Case Number : Case 1272 - 08 May Posted By: Guest
Please read the clinical history and view the images by clicking on them before you proffer your diagnosis.
Submitted Date :
F54. 1 year rash on right thigh not responding to antifungals. Worse with steroids. ?tinea incognito ?what
Case posted by Dr Richard Carr
Case posted by Dr Richard Carr


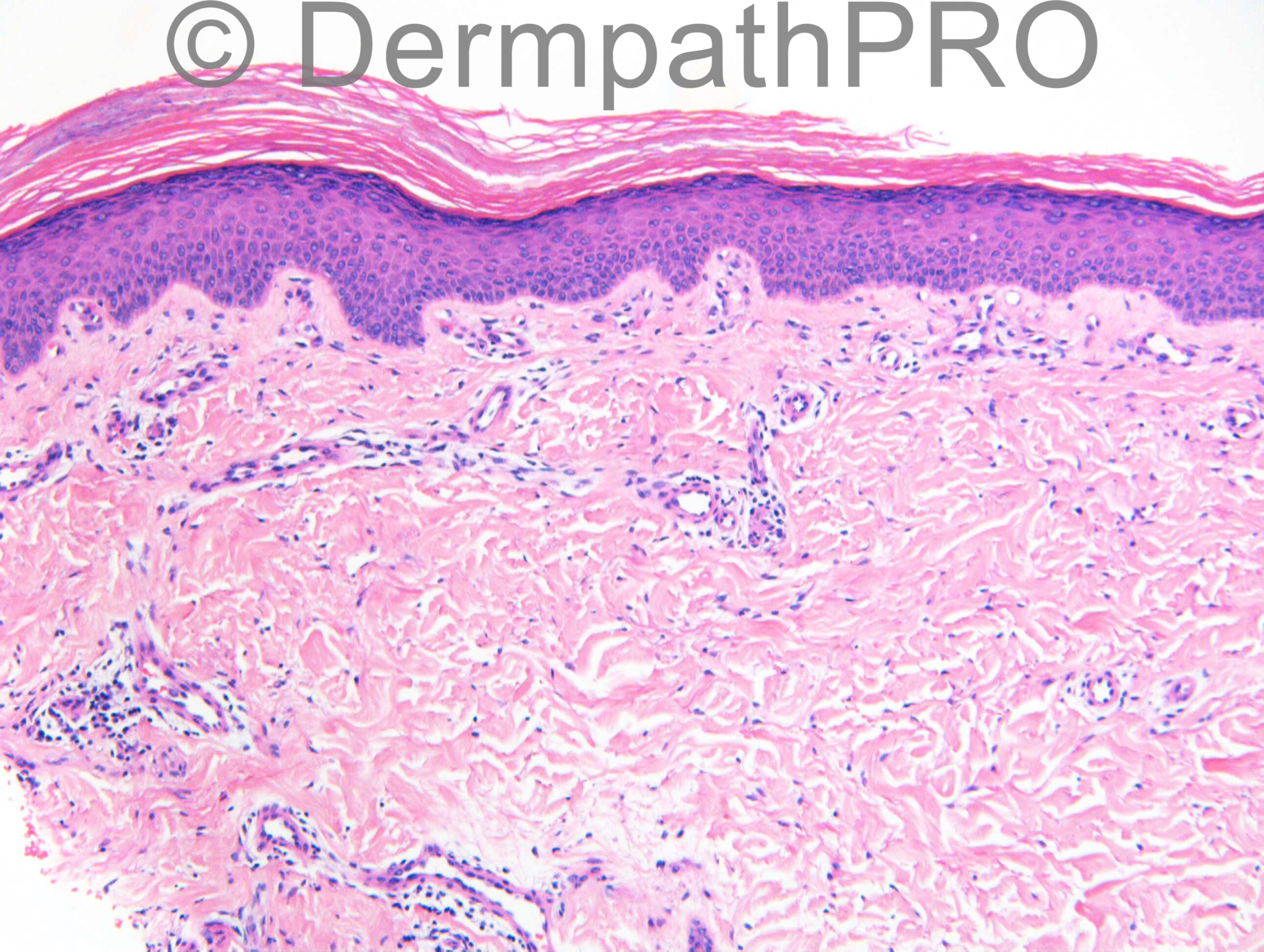
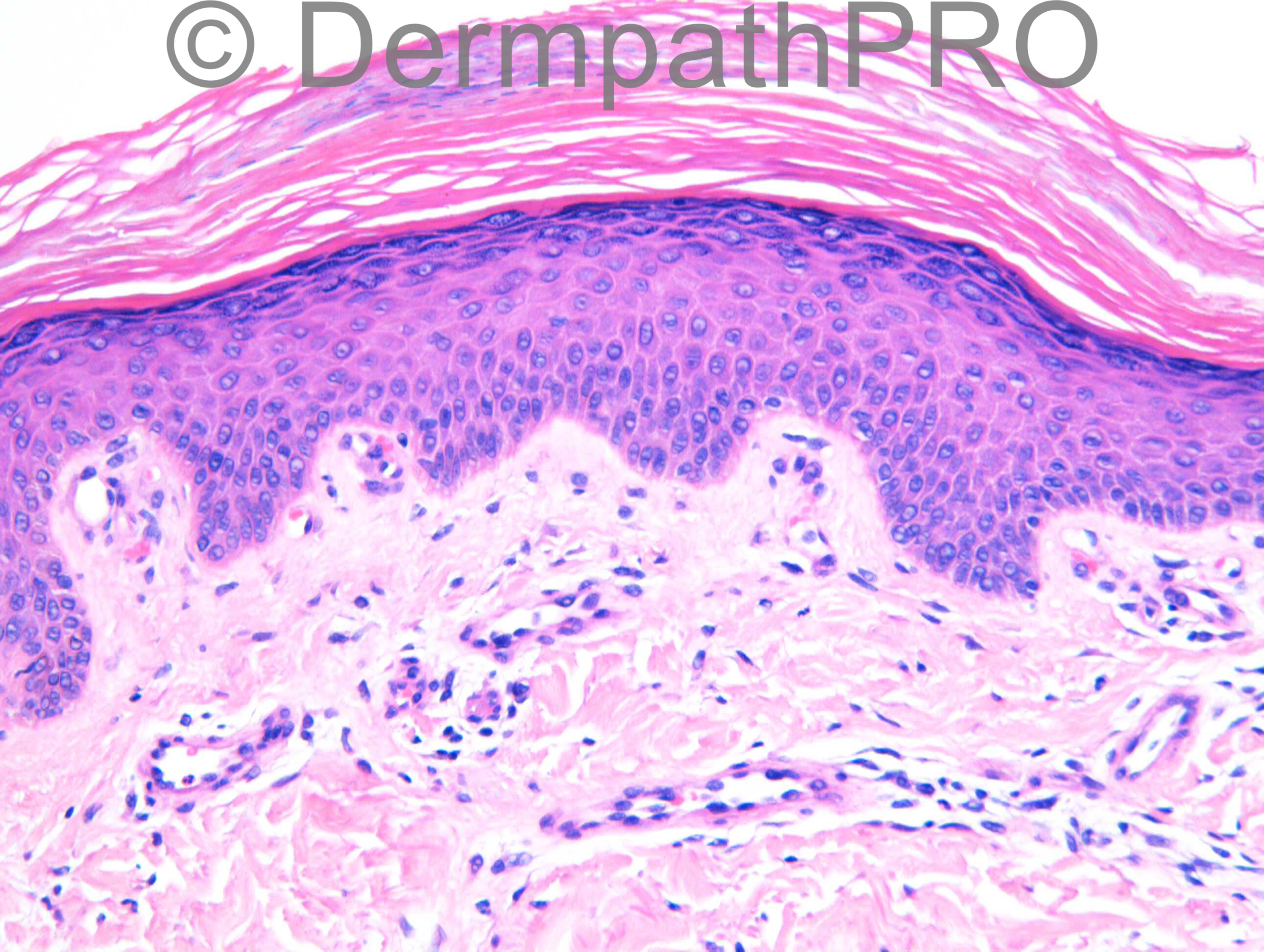
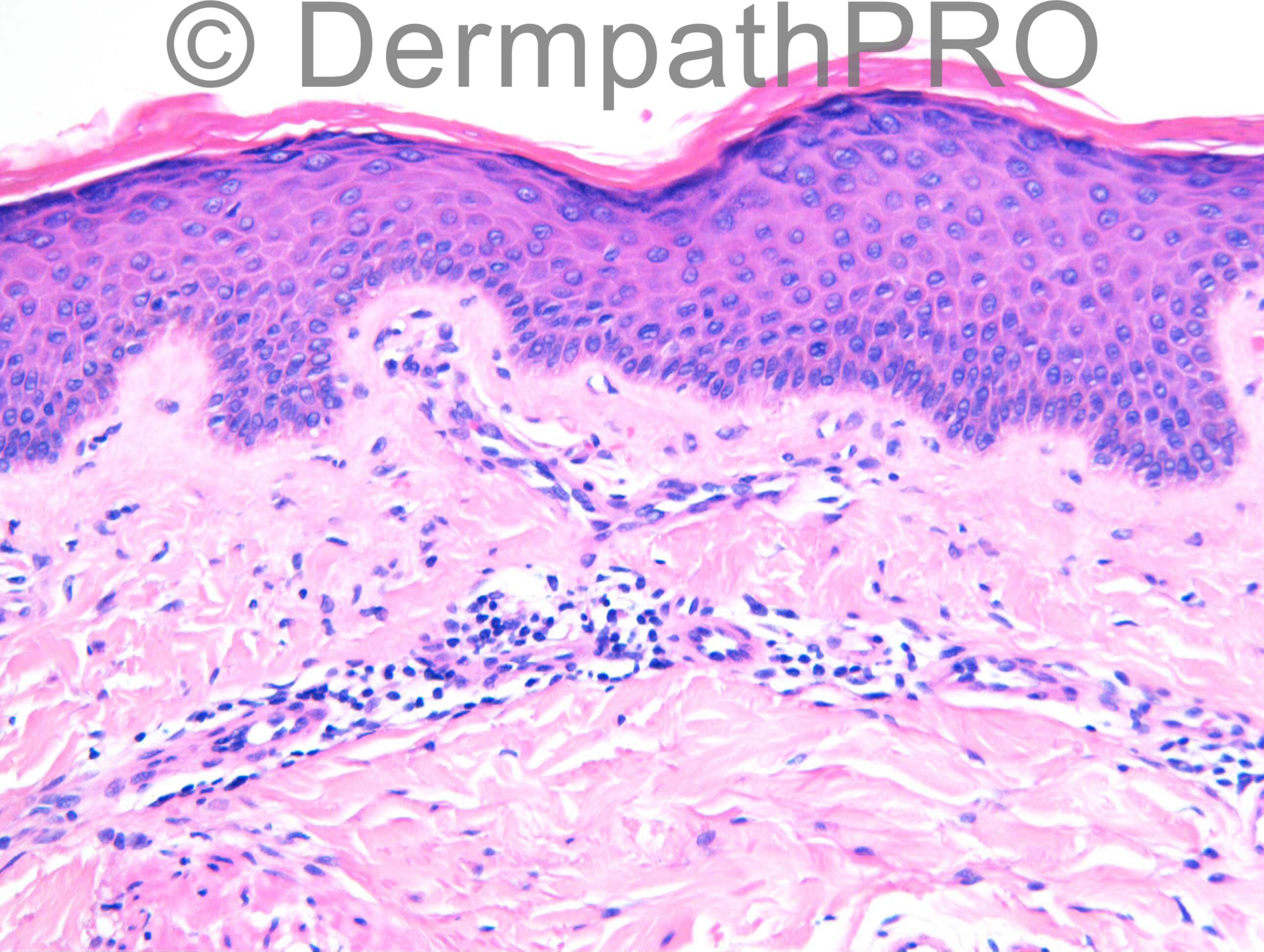

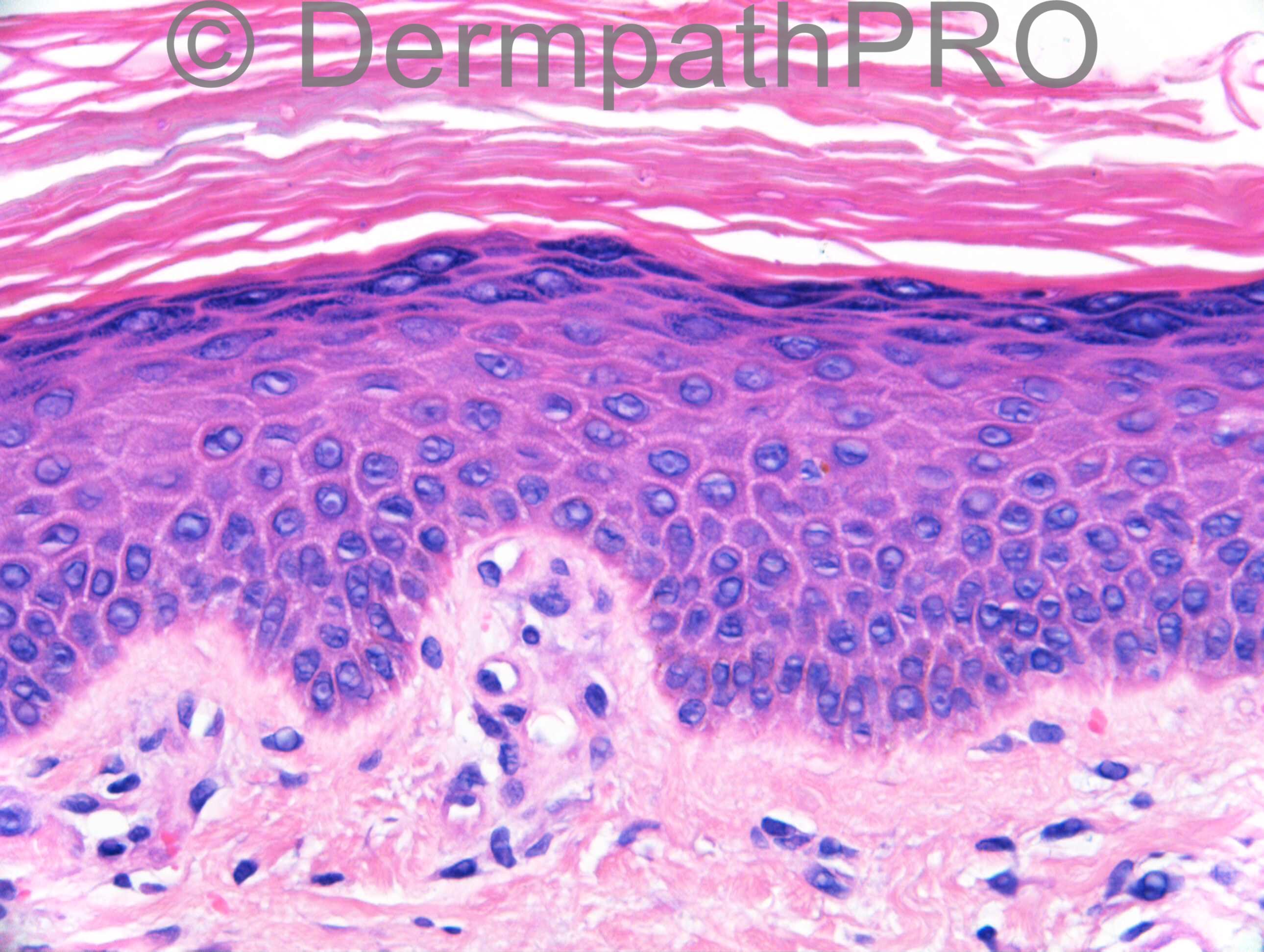
Join the conversation
You can post now and register later. If you have an account, sign in now to post with your account.