-
 1
1
Case Number : Case 1515 - 14 April Posted By: Guest
Please read the clinical history and view the images by clicking on them before you proffer your diagnosis.
Submitted Date :
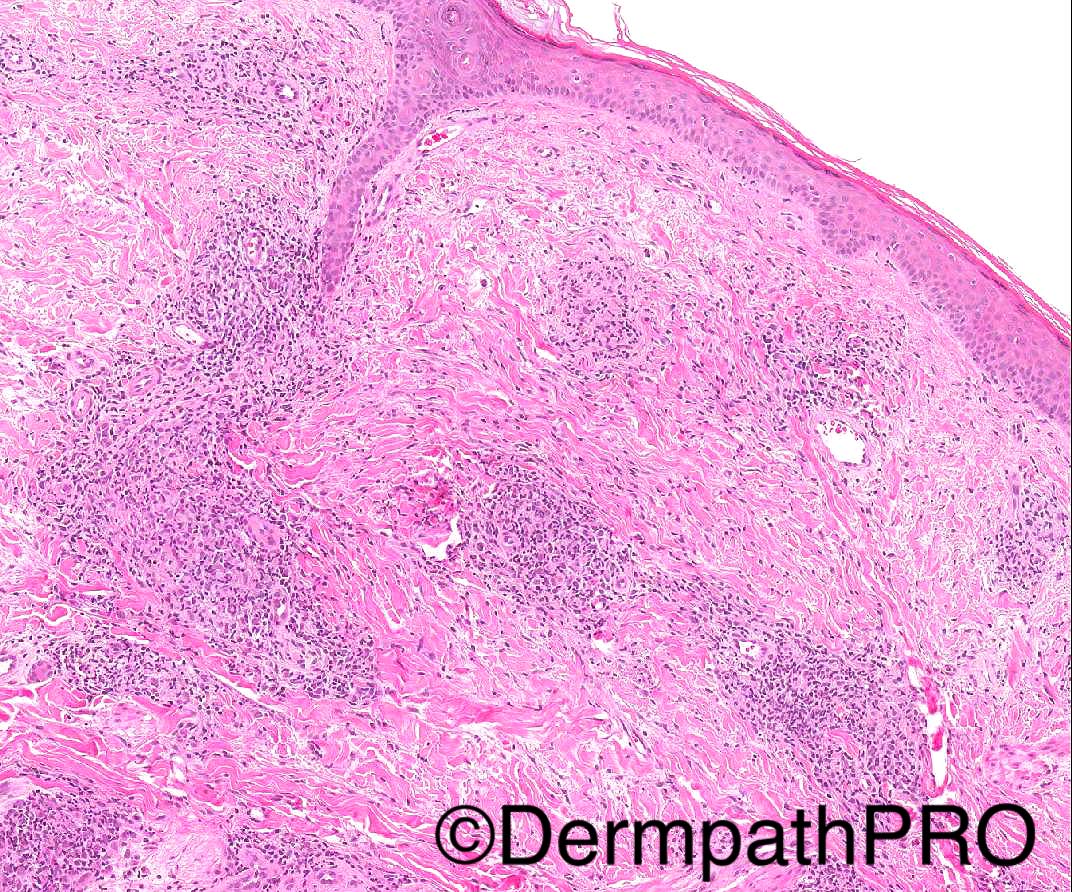
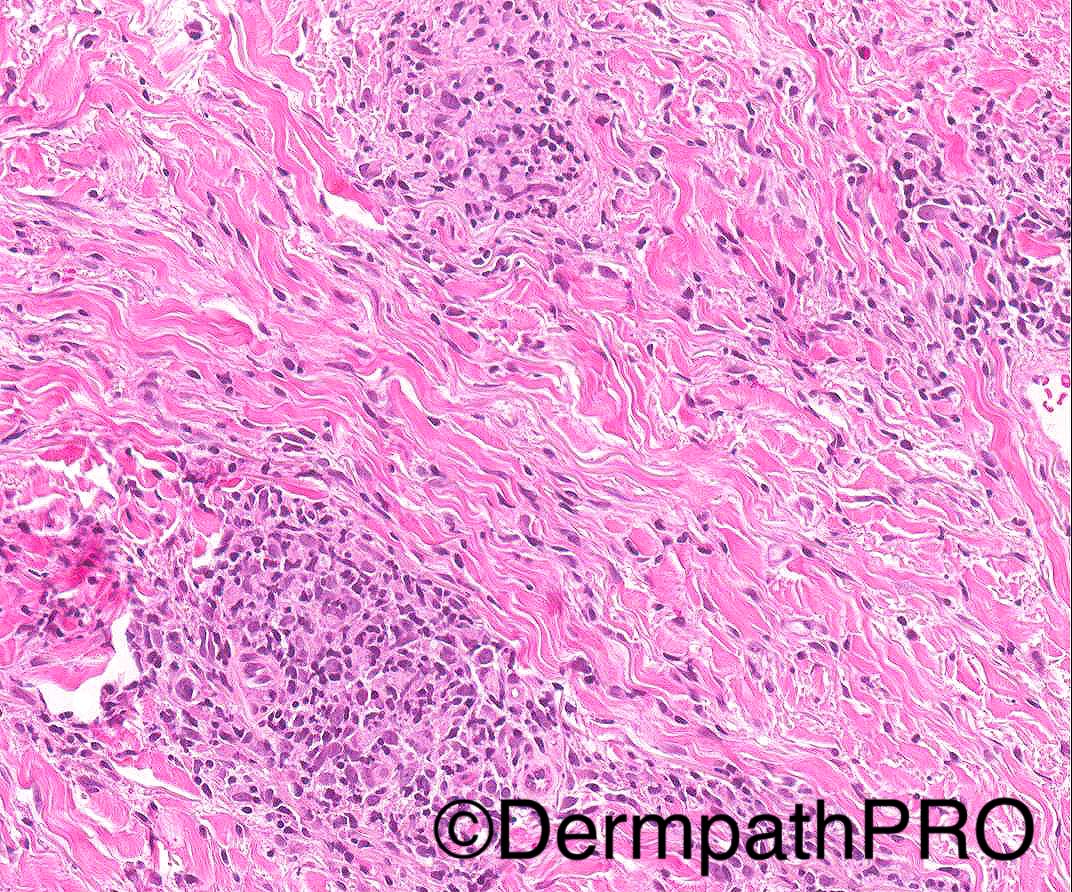
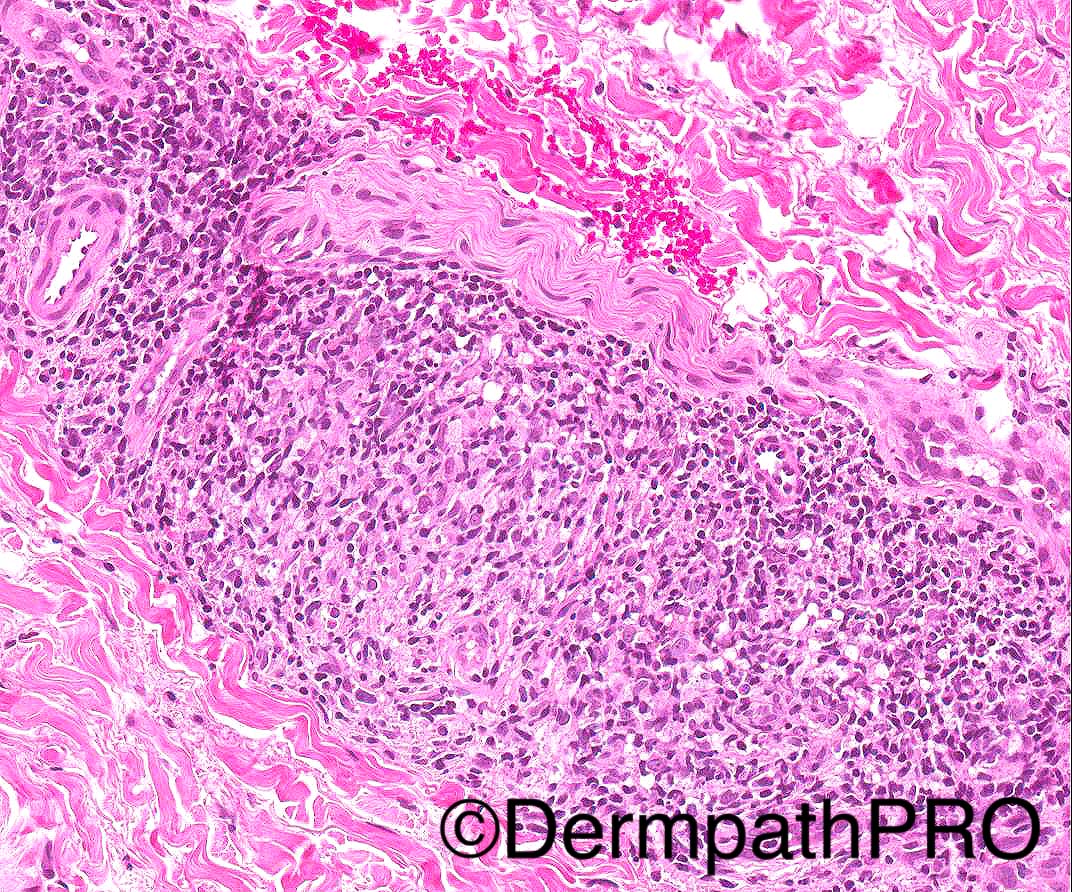
34/M widespread discrete plaques, some indurated.
PMH- recurrent chest infections and bronchiectasis, hepatosplenomegaly (splenectomy done in 2014), lymphadenopathy
- Special stains for AFB and fungi negative.
Case posted by Dr Arti Bakshi
PMH- recurrent chest infections and bronchiectasis, hepatosplenomegaly (splenectomy done in 2014), lymphadenopathy
- Special stains for AFB and fungi negative.
Case posted by Dr Arti Bakshi



Join the conversation
You can post now and register later. If you have an account, sign in now to post with your account.