Edited by Admin_Dermpath
Case Number : Case 1647 - 18 October Posted By: Guest
Please read the clinical history and view the images by clicking on them before you proffer your diagnosis.
Submitted Date :
F80. Forearm lesion. Viral wart?
Case Posted by Dr Richard Carr
Case Posted by Dr Richard Carr

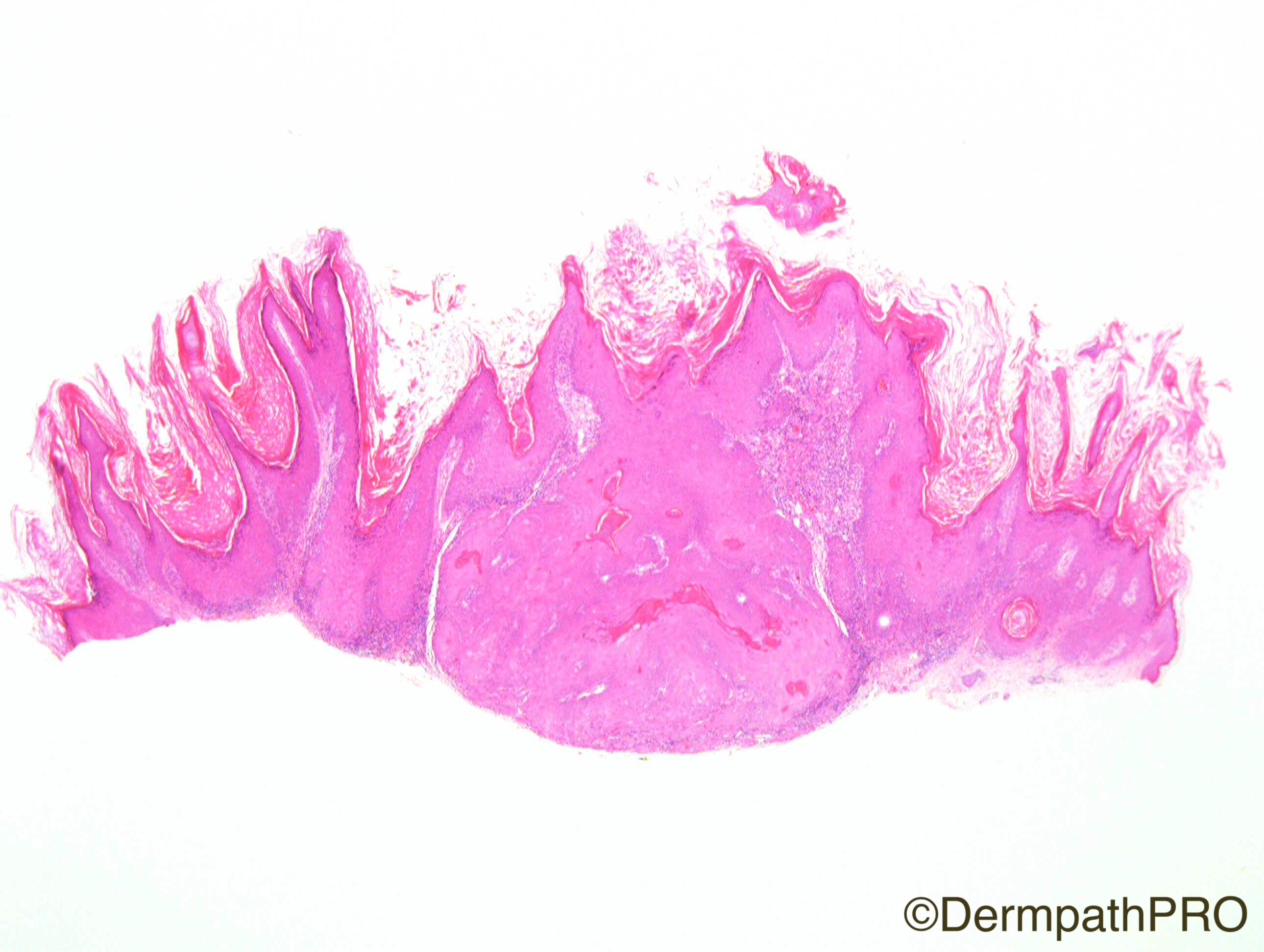
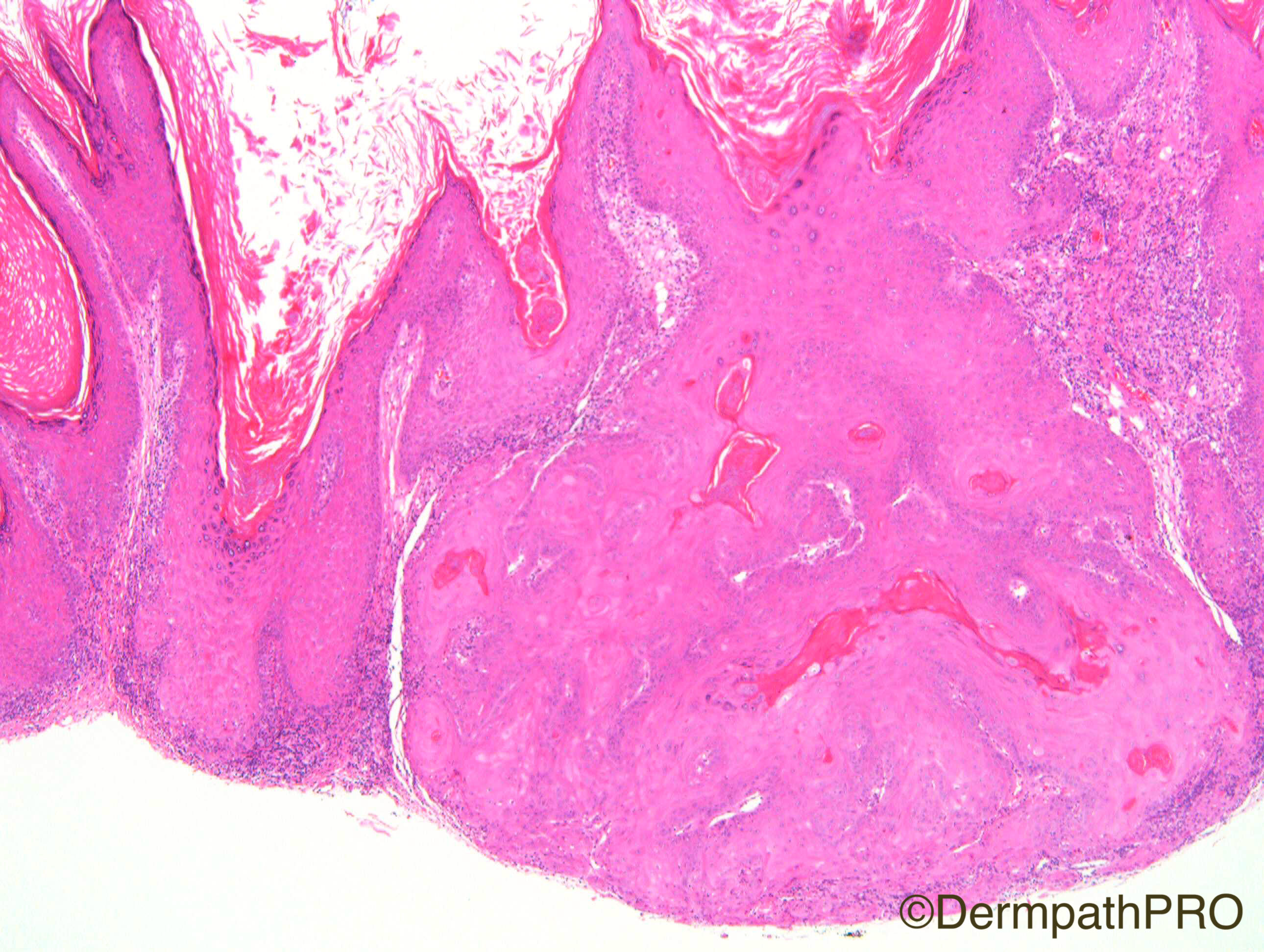
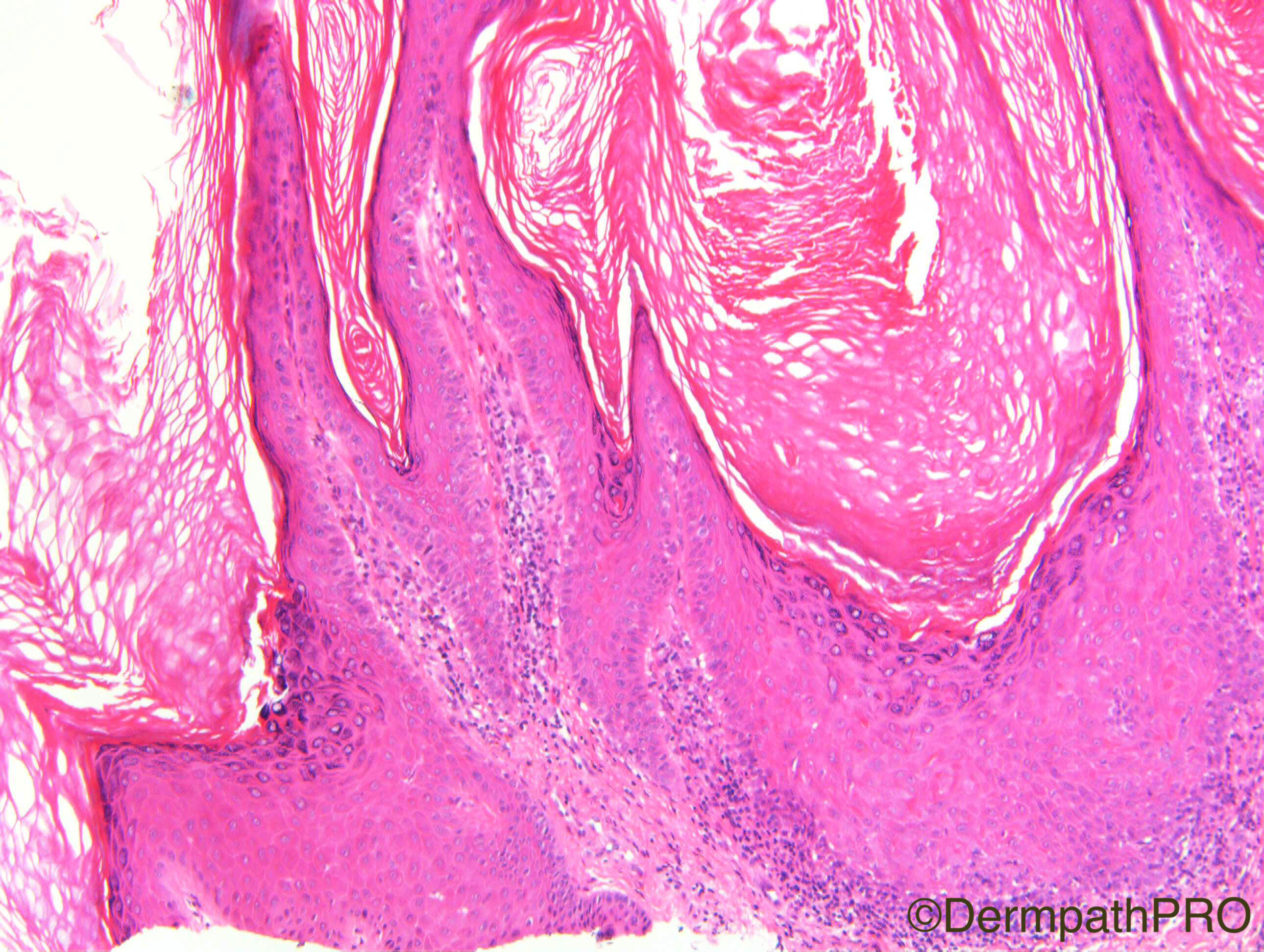
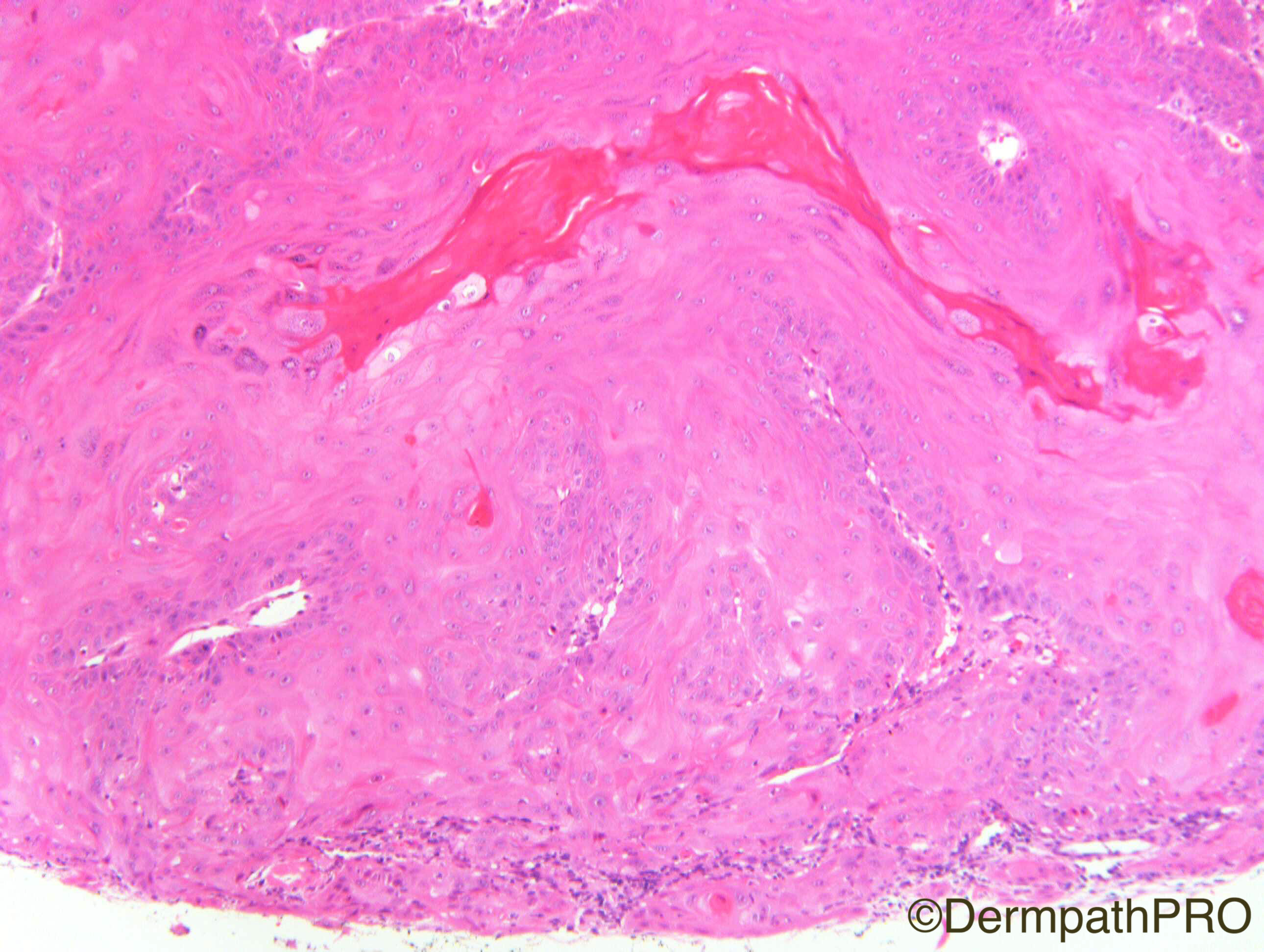
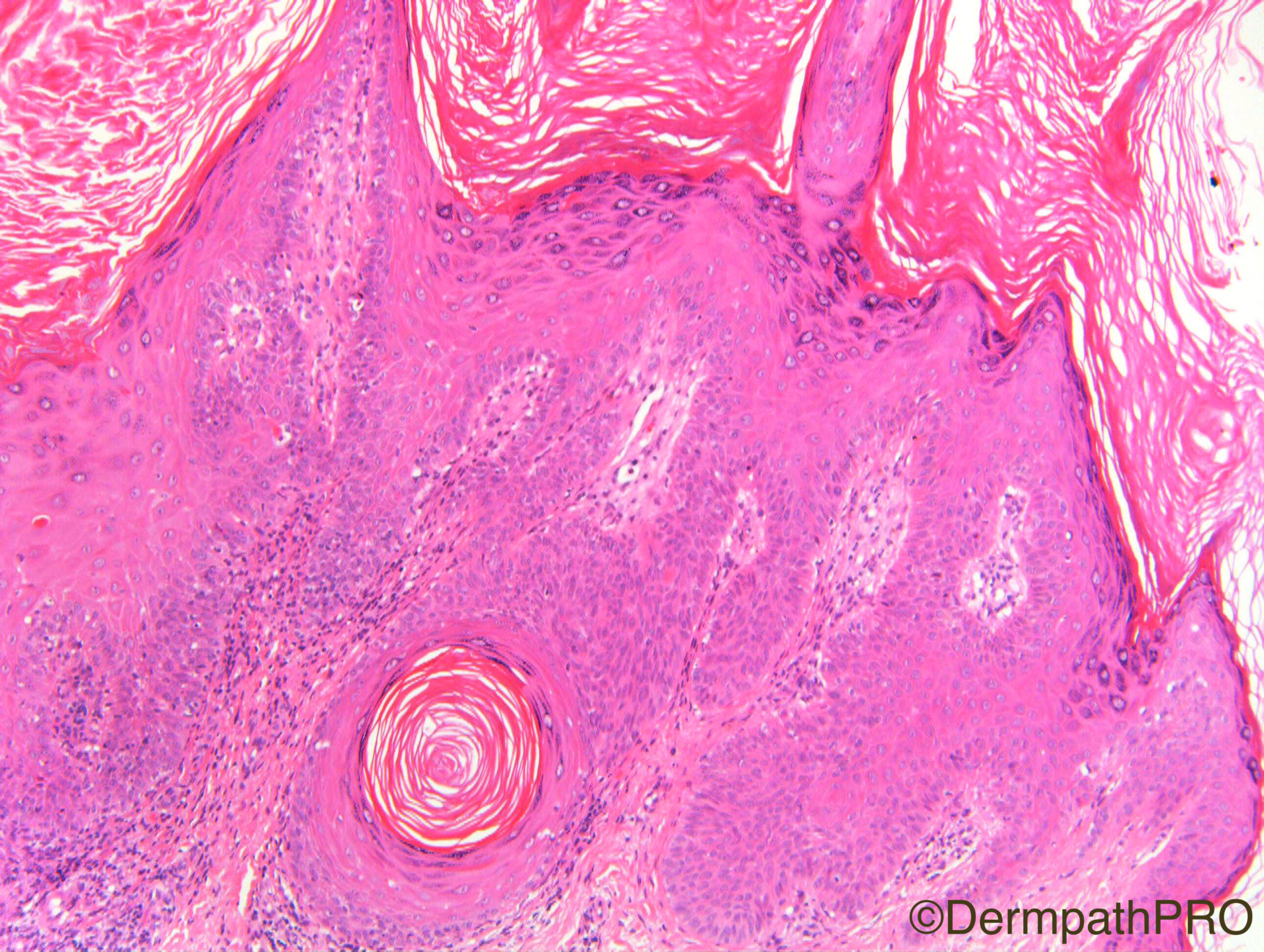
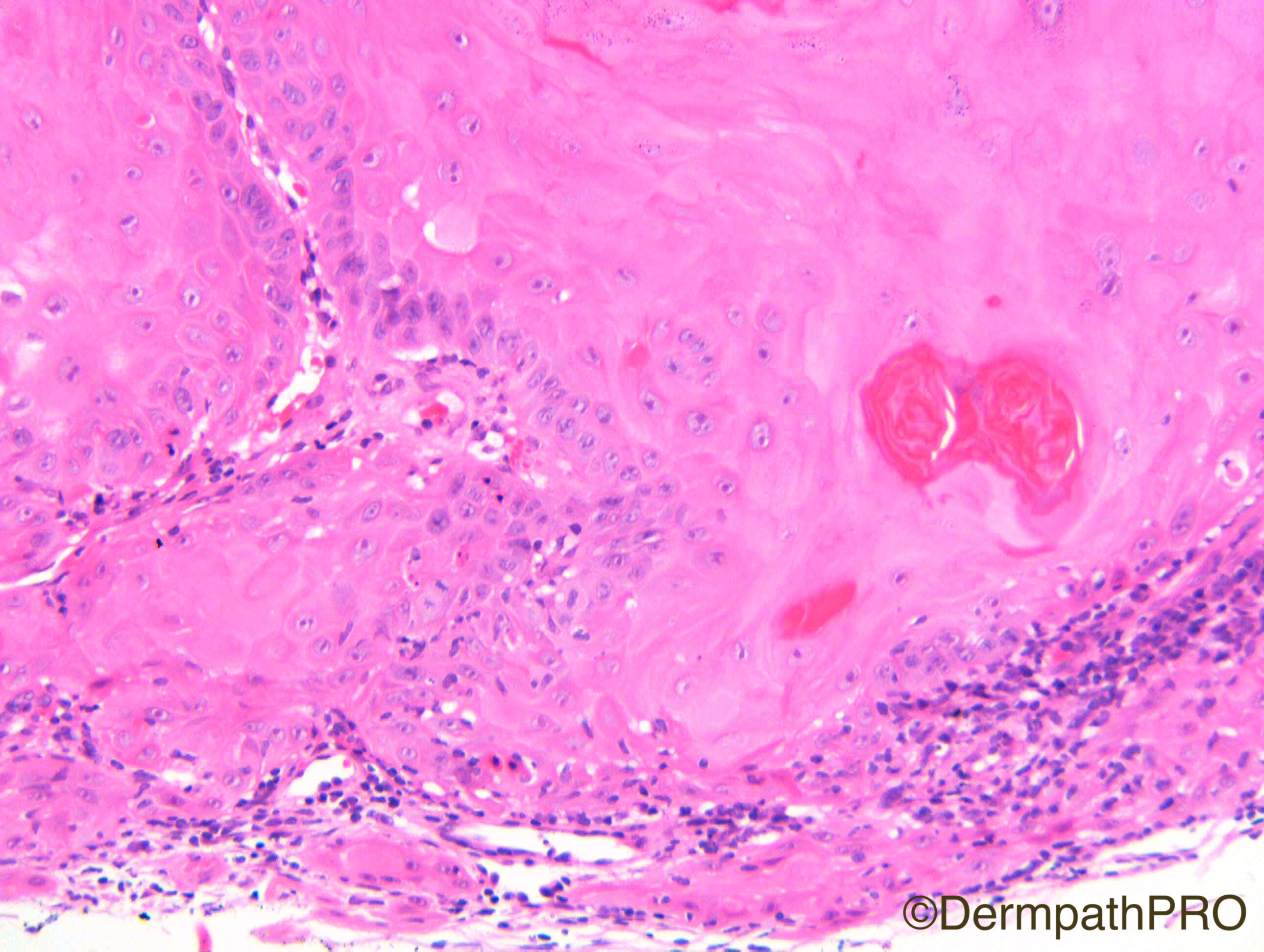
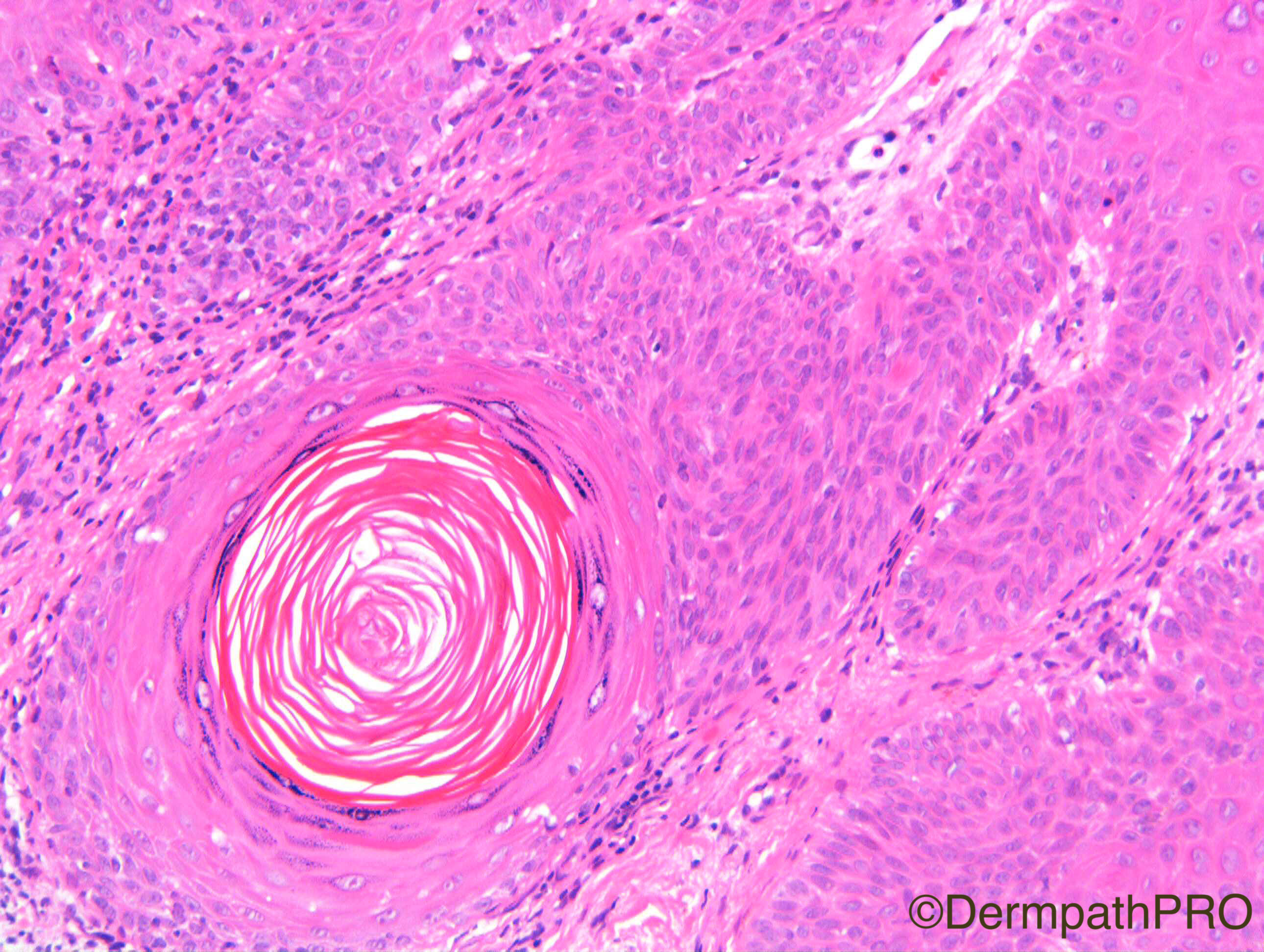
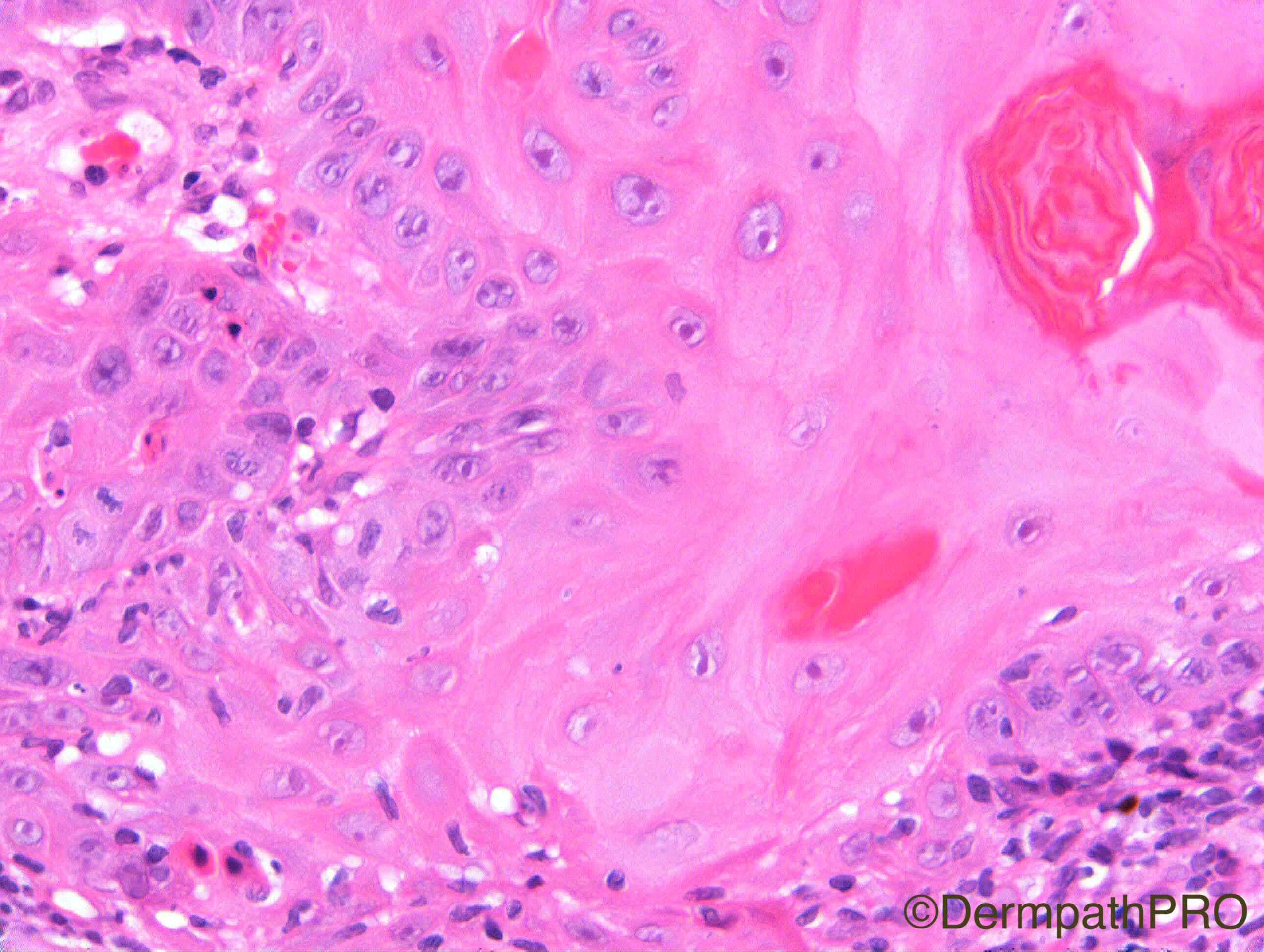
Join the conversation
You can post now and register later. If you have an account, sign in now to post with your account.